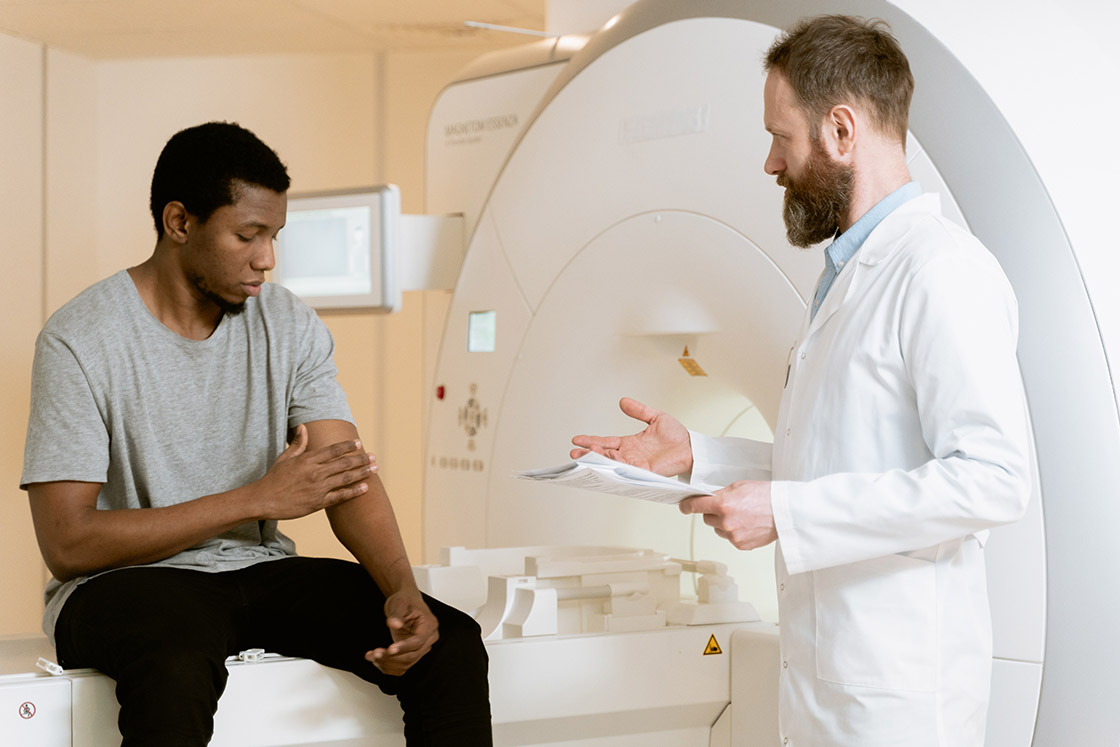
In medicine, there is a long tradition of starting case presentations with a three-part description of the patient’s age, sex, and race: “this 53-year-old White woman presented to the ER with abdominal pain” or “the patient is a 50-yearold Black man with chest pain.”
In December 2021, two doctors wrote a perspective article in The New England Journal of Medicine questioning that practice. Allan Brent, MD, and Christopher Goodman, MD, wrote: “Given persistent racism in medicine and the growing recognition that racial and ethnic categories are socially constructed and not biologically coherent, the practice of mentioning race or ethnicity immediately in case presentations—alongside age and sex—is worth revisiting.”
They made some excellent points, and a vigorous discussion ensued in the online comments and in letters to the editor that were printed in the Journal. One recommended that educators also consider the way a patient’s disability is described, because it can create assumptions and bias diagnostic and treatment decision making.
Another letter referenced a study on “Racial bias in presentation of cases” in which the authors found that race was specified more often during presentations of Black than of White patients. The authors wrote: “Race was more often specified prominently and repeatedly during presentations of Black patients. Among patients to whom ‘possibly unflattering’ characteristics were attributed, race was more likely to be specified for Blacks (10 of 10) than for Whites (4 of 9).” They commented that these case presentations appeared to show a subtle bias.
Another letter to the editor asked, “who determines the patient’s race and on what basis?” (a good question, since there is no scientific basis) and objected to stating that certain diseases are more common in certain racial groups (e.g., cystic fibrosis in White patients or sickle cell anemia in Black patients) because it “adds to the misinterpretation that racial groups are biologically determined.” The writer describes the complaints he got twenty years ago for a case study involving a Black teenager with night blindness caused by vitamin A deficiency due to cystic fibrosis. Readers objected that Blacks don’t get cystic fibrosis, that if they do it’s too rare to mention, and that the example just confused students. A gastroenterologist said, “It is rare that a teenager has pancreatic insufficiency, but whatever their race, the most common reason for pancreatic insufficiency in teens is cystic fibrosis.” The writer commented, “I appreciate that one way to address part of the racial disparity in U.S. health care is to target conditions that more often affect racial groups other than White Americans, but physicians should be treating the patient, not the race.” I couldn’t agree more.
I noticed that many of the online commenters thought the article was saying that race should be ignored. That’s not what it said at all. It was only arguing against putting race in the headlines. It said, “clinically relevant and patient-specific socioeconomic considerations, cultural beliefs, and race-related barriers to high-quality health care should be acknowledged and addressed later in the case presentation.” And: “Later in the case presentation, clinicians can review strong associations between suspected diagnoses and ancestral groups and can propose appropriate testing for genetic or biologic markers—on the basis of all clinically relevant information and not simply race or ethnicity.”
Several commenters recommended the patient be humanized as an individual in the audience’s minds. Some thought race was an essential component of the patient’s identity; others thought it might be more appropriate to mention that the patient was a World War II veteran and an avid chess player. One said we shouldn’t suppress our biases but should confront them and deal with them. No one suggested a thought I had: using the patient’s first name would both help bring him to life as a real person and would demonstrate intimacy, understanding, and respect for the individual.
One commenter suggested that it should be the patient who decides how their case is presented. Several mentioned conditions where the incidence or response to treatment varies by race. They thought mentioning race improved diagnosis, but one commenter said he had stopped mentioning race in his initial descriptions because it added nothing to his diagnostic considerations. One commenter thought it was naïve to pretend that race and/ or ethnicity don’t exist. One said affirmative action was racist and that it had achieved its goal in that “White males have been essentially ethnically cleansed from medicine.” Others called the article nonsense and evidence of cancel culture and of the intrusion of politics and wokeism into medicine.
What is Race?
Race and ethnicity are often confused. Race tends to emphasize physical characteristics like skin color, while ethnicity reflects factors like geography, history, culture, and religion. Racial and ethnic groups are not static. They are fluid and evolve over time.
Unlike sex and age, which are verifiable facts, race is a more fluid social construct. You might say it’s in the eye of the beholder. Barack Obama was criticized both for being too Black and for not being Black enough. When a man told my friend Susan he had voted for Obama because he was Black, she replied that she had voted for Obama because he was White.*
In 2022, the American Association of Biological Anthropologists issued a statement on race and racism. It explains that there is more variation within a race than between races. “Race” is an arbitrary and artificial division of populations into units based on historical contexts and social, cultural, and political motives. “Populations,” rather than “races,” is a more accurate descriptor. “The belief in races as a natural aspect of human biology and the institutional and structural inequities (racism) that have emerged in tandem with such beliefs in European colonial contexts are among the most damaging elements in human societies.”
“Race” is an arbitrary and artificial division of populations into units based on historical contexts and social, cultural, and political motives.
The “one-drop rule” asserted that having a single Black ancestor any time in the past, however distant (one drop of Black blood), meant a person was Black. The legal definition of race varied by state. Thomas Jefferson’s children with his slave Sally Hemings were legally White under Virginia law because their ancestry was seven-eighths European, but they were also legally slaves because they were born to a slave mother.
Races are not “pure.” Increasing numbers of people have mixed ancestry and can’t be pigeon-holed. DNA analysis has found that the average African-American genome is nearly a quarter European, and almost four percent of Americans who thought their ancestors were all European actually have African ancestors.
While race is not based on biology, it has real biological consequences for medical care, diagnosis, and treatment. Racial minorities have long been second-class citizens and have suffered abuses like the unethical Tuskegee syphilis study that denied effective treatment to Black men. As a result, a hundred of them died when they shouldn’t have. Minorities are often underrepresented in scientific studies, and diseases that are more common in minorities are less likely to be studied.
Medical Disorders in Racial and Ethnic Groups
None of this is to deny that certain disorders are more common in certain racial and ethnic groups, or populations:
- Cystic fibrosis in people of Northern European ancestry.
- Sickle cell anemia in people whose ancestors were from sub-Saharan African and certain south European countries.
- Thalassemia in people with Mediterranean ancestry.
- Hemochromatosis in European populations.
- Tay-Sachs disease in Ashkenazi Jews and a few other groups.
There are others.
But these diseases are not strictly limited to those racial and ethnic groups. Doctors can be misled if they fail to consider the disease in a patient who does not belong to the group or if they commit to a diagnosis prematurely because of its association with a patient’s race or ethnicity. Racial self-identification can be unreliable due to factors like undetected adultery and unreliable memory.
Many common chronic diseases like diabetes and heart disease are multifactorial and their prevalence is affected by both genetic and environmental factors, making it difficult to identify the influence of “race.” The typical progress of a disease may differ in different racial and ethnic groups, but that doesn’t mean the cause is genetic; it could be social or environmental.
Sometimes treatment is based on race. Bidil, a drug for congestive heart failure, was licensed for patients who self-identified as Black. Its approval was controversial. Critics objected that the data did not show it was more effective in Blacks than in Whites, only that it was more effective for Blacks than other similar drugs. Some called the licensing a race-based advertising scheme.
Racism Persists in Society and in Medicine
The U.S. has made a lot of progress since the days of lynching and segregation. Things are much better than they were, but we have a lot of progress left to make.
We would like to believe that doctors are color-blind, but there is plenty of evidence to the contrary. I would argue that we are all prejudiced to some degree by our personal experiences and the influence of others. The trick is to be aware of the possibility of bias and guard against letting it influence our behavior.

This article appeared in Skeptic magazine 27.3
Buy print edition
Buy digital edition
Subscribe to print edition
Subscribe to digital edition
Download our app
Brent and Goodman, authors of the aforementioned NEJM article, note that “routine inclusion of race or ethnicity at the beginning of a case presentation reinforces the still-prevalent but mistaken belief that race or ethnicity is a robust surrogate for genetic or innate biologic predisposition to disease.” So, obviously the way cases are presented contributes to false beliefs about race, and the current practice should be re-evaluated.
What if a patient with a broken arm is an unemployed, uninsured, homeless single mother of two toddlers who has been sleeping in a car with her children? What if she is HIV positive and has high blood pressure and is not getting treatment? Does it matter what her race is? Absolutely not! Whether she is black, white, yellow, or chartreuse, her treatment needs are the same: a cast for her arm, anti-retroviral and anti-hypertensive drugs, and social assistance. It may be important to know her race at some point, but that can wait. First things first! ![]()
*Barack Obama was the first biracial President of the United States. In his 2008 campaign speech in Philadelphia he famously said: “I am the son of a Black man from Kenya and a White woman from Kansas.”
About the Author
Harriet Hall, MD, the SkepDoc, is a retired family physician, former flight surgeon, and retired Air Force Colonel who writes about medicine, pseudoscience, alternative medicine, quackery, and critical thinking. She is a contributing editor and regular columnist for both Skeptic and Skeptical Inquirer magazines and an editor at ScienceBasedMedicine.org, where she has written an article every Tuesday since its inception in 2008. She wrote the book Women Aren’t Supposed to Fly: The Memoirs of a Female Flight Surgeon. The full texts of all her many hundreds of articles can be read on her website www.skepdoc.info.
This article was published on November 15, 2022.